
The creation and management of psychiatric progress notes are a cornerstone of effective patient care within the mental health field. These detailed records provide a comprehensive overview of a patient's condition, treatment plan, and progress, facilitating collaboration among providers, caregivers, and the patient themselves. A well-structured psychiatric progress note template is not merely a document; it's a vital tool for ensuring continuity of care and promoting positive outcomes. Psychiatric Progress Note Template is a standardized format designed to capture essential information, promoting clear communication and accountability. This article will delve into the key components of a robust psychiatric progress note, exploring its importance, best practices, and variations to suit different clinical settings. Understanding how to effectively utilize this template can significantly improve the quality of care delivered to individuals experiencing mental health challenges.
The Importance of Psychiatric Progress Notes
The initial implementation of psychiatric progress notes revolutionized the way mental health care was delivered. Prior to this, fragmented information often existed, leading to inconsistent assessments and potentially suboptimal treatment. Today, the standardized format allows for a holistic view of a patient's experience, fostering a more collaborative and data-driven approach. The benefits extend beyond simply documenting events; they contribute to improved patient engagement, enhanced communication, and ultimately, better clinical outcomes. Psychiatric Progress Note Template is increasingly recognized as a critical component of evidence-based practice, driving improvements in patient satisfaction and overall care quality. Furthermore, the use of these notes facilitates regulatory compliance and data analysis, supporting quality improvement initiatives within healthcare systems.
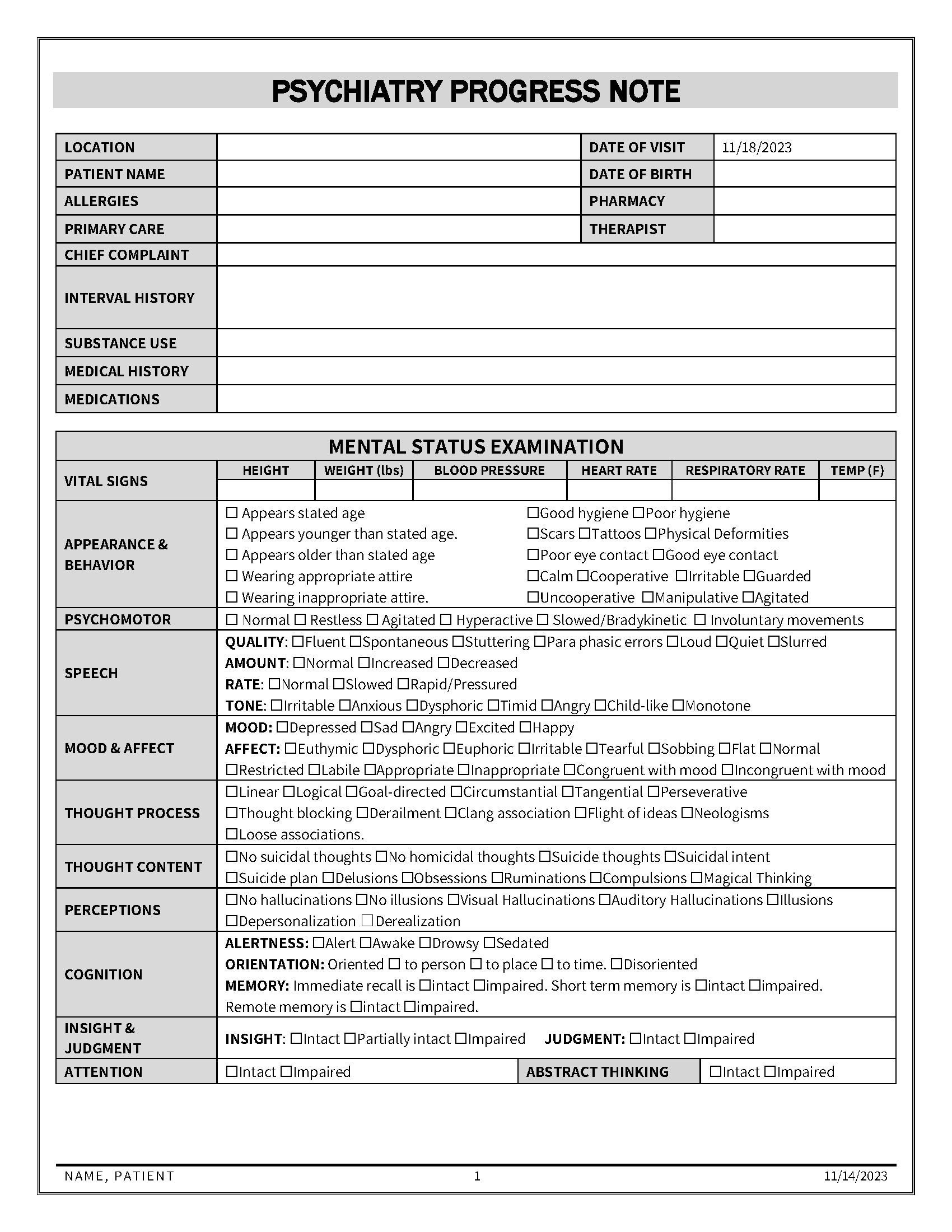
Core Components of a Psychiatric Progress Note
A comprehensive psychiatric progress note typically includes several key sections, each addressing a specific aspect of the patient's care. The precise format may vary slightly depending on the institution and the clinician's preferences, but the core elements remain consistent. Here's a breakdown of the essential components:
1. Patient Demographics & Initial Assessment
This section provides essential information about the patient, including their name, date of birth, contact information, and a brief summary of their initial presentation. It also includes a preliminary assessment of their mental state, including any immediate concerns or symptoms. Psychiatric Progress Note Template begins with a clear identification of the patient's current situation, highlighting any significant changes or concerns. This initial assessment forms the foundation for subsequent data collection.
2. Current Symptoms & Functional Status
This section meticulously details the patient's current symptoms, both physical and psychological. It's crucial to describe the nature and severity of these symptoms, using objective observations whenever possible. Furthermore, it assesses the patient's functional status – their ability to perform daily activities, such as maintaining hygiene, self-care, and social engagement. This section often incorporates standardized symptom scales (e.g., PHQ-9 for depression, GAD-7 for anxiety) to provide a quantifiable measure of their condition. Psychiatric Progress Note Template emphasizes the importance of capturing both subjective experiences and objective measures.

3. Treatment Plan & Interventions
This section outlines the treatment plan currently in place, including medications, therapy modalities (e.g., CBT, DBT), and other interventions. It should clearly state the rationale for each intervention and the patient's response to it. It also documents any changes to the treatment plan and the reasons for these changes. Psychiatric Progress Note Template requires a detailed record of all interventions delivered, including frequency, duration, and patient feedback.

4. Progress & Response to Treatment
This is arguably the most important section of the note. It provides a chronological record of the patient's progress over a specified period (e.g., one week, one month). It includes observations regarding the patient's response to treatment, including any improvements, setbacks, or changes in symptoms. This section allows clinicians to assess the effectiveness of the treatment plan and make necessary adjustments. Psychiatric Progress Note Template encourages clinicians to document not just what happened, but how it's impacting the patient.

5. Social Support & Family Involvement
This section addresses the patient's social support system and any involvement of family members or caregivers. It's important to document the availability of support, any challenges faced, and any strategies employed to facilitate social engagement. Psychiatric Progress Note Template recognizes the crucial role of family support in maintaining patient stability and promoting recovery.

6. Relevant Medical History & Current Health Status
This section includes a brief overview of the patient's relevant medical history, including any co-existing conditions or medications. It also documents any current health concerns or changes in physical health status. Psychiatric Progress Note Template ensures that all relevant medical information is readily accessible to healthcare providers.

Best Practices for Psychiatric Progress Note Creation
Creating effective psychiatric progress notes requires adherence to specific best practices. These include:

- Clarity and Conciseness: Use clear, concise language and avoid jargon.
- Objectivity: Record observations objectively, avoiding subjective interpretations.
- Accuracy: Ensure all information is accurate and verified.
- Completeness: Include all relevant information, as outlined above.
- Timeliness: Complete the note promptly after each session or event.
- Standardization: Utilize a standardized template to ensure consistency across providers.
The Role of Technology in Psychiatric Progress Note Templates
While paper-based templates remain a viable option, technology is increasingly being integrated into psychiatric progress note creation. Electronic health records (EHRs) and mobile apps streamline data capture, improve accessibility, and facilitate data analysis. These tools allow for automated note-taking, enhanced data visualization, and improved communication among providers. However, it's crucial to ensure that technology is used to support clinical documentation, not replace it. Psychiatric Progress Note Template integration with EHR systems is becoming increasingly common, offering significant benefits for efficiency and data management.

Variations and Adaptations of Psychiatric Progress Note Templates
Recognizing that each patient and setting presents unique challenges, various variations of the psychiatric progress note template exist. Some common adaptations include:

- Crisis Notes: Specific sections are dedicated to documenting crisis events, including immediate safety concerns and interventions.
- Medication Reconciliation: A detailed record of all medications, dosages, and patient responses is essential.
- Special Populations Notes: Templates tailored for specific populations, such as children, adolescents, or individuals with complex mental health conditions.
- Remote Monitoring Notes: For patients receiving telehealth services, progress notes capture data collected remotely.
Conclusion
The psychiatric progress note template is a fundamental tool in the mental health care continuum. Its consistent structure, comprehensive coverage, and emphasis on data-driven assessment contribute significantly to improved patient outcomes. By understanding the importance of this template and adhering to best practices, clinicians can effectively document patient progress, facilitate collaboration, and ultimately, enhance the quality of care. Psychiatric Progress Note Template remains a vital component of evidence-based practice, demonstrating its enduring value in supporting mental health treatment. Continued refinement and adaptation of this template, alongside the integration of technology, will undoubtedly further optimize its effectiveness in the years to come.

0 Response to "Psychiatric Progress Note Template"
Posting Komentar